Oesophageal Cancer
Anatomy of the Oesophagus
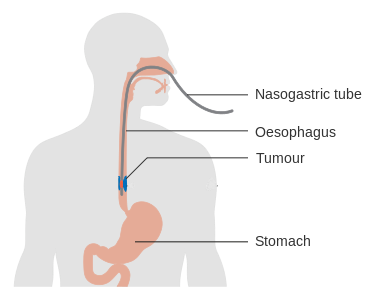
The oesophagus is the first section of the gastrointestinal tract.
It is a pink 20 cm muscular tube that extends from the throat to the stomach. It runs down behind the windpipe and heart and in front of the heart.
How the Oesophagus Works
The oesophagus has one core function: transferring food, liquids, and saliva from the mouth to the stomach.
Food is moistened and pushed into the stomach using different layers of tissue in the oesophagus (mucosa and muscle).
What is Oesophageal Cancer?
Oesophageal cancer is a cancerous growth in the cells lining the oesophagus, a tube connecting the throat to the stomach. This disease is a type of gastrointestinal cancer, and it is relatively rare compared to other types of cancer.
Impact of Oesophageal Cancer on Anatomy and Health
Oesophageal cancer can cause significant damage to the body, particularly if left untreated. The oesophagus is a vital organ that plays a critical role in digestion, and any damage to this organ can lead to severe health complications.
Cancer cells in the oesophagus can interfere with the organ's ability to function correctly. This can lead to problems with swallowing and digestion, as well as other symptoms such as chest pain, weight loss, and coughing.
Risk Factors for Oesophageal Cancer
Oesophageal cancer can affect anyone, but some people are at a higher risk than others. Some of the factors that can increase the risk of developing oesophageal cancer include:
- Age: 80% of people living with oesophageal cancer are over 60.
- Gender: Men are more likely than women to develop oesophageal cancer.
- Tobacco and heavy alcohol use
- Obesity
- Gastrointestinal disorders: Certain gastrointestinal disorders, such as gastroesophageal reflux disease (GERD)
- Family history
Causes of Oesophageal Cancer
The exact causes of oesophageal cancer are still unknown. Most are linked to lifestyle and environmental factors. Some factors that are associated with an increased risk of Oesophageal Cancer are:
- Genetic mutations: Changes in the DNA of the cells in the oesophagus can cause cancerous growths to form.
- Environmental factors: Exposure to certain chemicals and toxins, such as those found in tobacco smoke, can increase the risk of developing oesophageal cancer.
- Lifestyle factors: Certain lifestyle factors, such as heavy alcohol consumption and a high-fat diet, can increase the risk of developing oesophageal cancer.
- Medical conditions: Certain medical conditions, such as gastro-oesophageal reflux disease (GORD) and Barrett's oesophagus, can increase the risk of developing oesophageal cancer.
Symptoms of Oesophageal Cancer
The symptoms of oesophageal cancer can vary depending on the stage of the disease. In the early stages, the symptoms may be minimal or non-existent, making it difficult to detect the cancer. As the cancer progresses, however, the symptoms become more noticeable and may include the following:
- Difficulty swallowing (dysphagia): pain or a burning sensation when swallowing, or your food may stick in your throat
- Acid indigestion or heartburn: when acid from the stomach goes back up (refluxes) that is persistent or lasts more than three days, or if the stomach becomes inflamed or irritated
- Weight loss
- Regurgitation or vomiting: when food comes back up soon after you swallow it
- Pain in your throat or behind your breastbone: pain in the centre of your chest or, more rarely, in your back or shoulder
- Hoarseness: voice can become raspy or croaky
- Chronic cough: cough that won't go away or that happens when you try to eat
- Coughing up blood or blood in your vomit
- Dark faeces
Types of Oesophageal Cancer
There are two main types of oesophageal cancer: squamous cell carcinoma and adenocarcinoma.
- Squamous cell carcinoma is a type of cancer that begins in the thin, flat cells lining the oesophagus. This type of cancer is more common in people who smoke or drink alcohol heavily.
- Adenocarcinoma: A type of cancer that begins in the cells that produce and release mucus in the oesophagus. This type of cancer is more common in people who have Barrett's oesophagus, a condition in which the cells in the lower part of the oesophagus change due to repeated exposure to stomach acid.
Preventing Oesophageal Cancer
While not all cases of oesophageal cancer can be prevented, many of the known risk factors can be reduced through healthy lifestyle choices and early medical management of related conditions. Preventive strategies focus on protecting the lining of the oesophagus from chronic irritation and inflammation, which over time may increase the risk of cancer development.
- Manage Chronic Acid Reflux (GERD)
- Maintain a Healthy Body Weight
- Stop Smoking
- Limit Alcohol Consumption
- Eat a Healthy Diet
- Regular Medical Monitoring for High-Risk Individuals
- Avoid Chronic Irritation to the Oesophagus
Diagnosis of Oesophageal Cancer
Oesophageal cancer is typically diagnosed through a combination of tests and procedures. Some of the most common diagnostic tools include:
- Endoscopy: A thin, flexible tube with a camera is inserted through the mouth and into the oesophagus to look for abnormal areas.
- Biopsy: A tissue sample is taken from the oesophagus during endoscopy and examined under a microscope for cancer cells.
- Imaging tests: X-rays, CT scans, and PET scans can help determine the stage and location of the cancer.
- Blood tests: Blood tests can detect certain markers that may indicate the presence of oesophageal cancer.
Tests After Diagnosis
Once a diagnosis of oesophageal cancer is made, further tests will be required. These tests are necessary to define cancer’s size, position, stage, and spread. They do not always answer with certainty what stage the cancer is. Only after surgery can further answers be found. These tests may include the following:
- CT scan
- Endoscopic ultrasound (EUS)
- PET-CT
- Laparoscopy
- MRI
Stages of Oesophageal Cancer
The cancer stage tells you how big it is and how far it’s spread. Staging is an important part of oesophageal cancer diagnosis, as it helps doctors determine the best course of treatment. The stages of oesophageal cancer or tumours are:
- Stage 1 - within the oesophageal tissue
- Stage 2 - grown into the wall of the oesophagus
- Stage 3 - moved to the outer oesophageal wall
- Stage 4 - expanded to one or more organs or structures near the oesophagus
- metastasised to the lungs, heart or rib cage tissue
- metastasised to the windpipe, spine or major blood vessel
Other important measurements used to determine the progression of the cancer are:
- the spread to lymph nodes
- the extent of metastasis
- the grade or cell patterns under a microscope.
Treatment for Oesophageal Cancer
A patient’s treatment and survival rate for oesophageal cancer mainly depend on the cancer's stage and location. The doctor can advise after diagnosis and surgery. There are several treatment options available for oesophageal cancer, including:
- Surgery: Involves removing part or all of the oesophagus and nearby lymph nodes. This is typically the preferred treatment for early-stage oesophageal cancer.
- Chemotherapy: Involves using powerful drugs to kill cancer cells. This treatment is typically used in combination with surgery or radiation therapy.
- Radiation therapy: Uses high-energy radiation to kill cancer cells. This treatment may be used before or after surgery or with chemotherapy.
Oesophageal Cancer Surgery
A cure for oesophageal cancer is sometimes possible through surgery. Surgery removes cancer, sometimes along with part of the oesophagus and other affected tissue. Your surgeon can offer various operations depending on
- where your cancer is
- the stage
- the type of oesophageal cancer
- the grade
- patient's general health and fitness
Some surgical approaches include:
- Endoscopic Mucosal Resection: Very early-stage cancer is removed through an endoscope. This can be a day procedure with a fast recovery.
- Oesophagectomy: The affected oesophageal sections are removed, and where necessary, parts of the upper stomach, lymph nodes and other tissue. The oesophagus is then reconnected to the gastrointestinal tract.
Oesophageal Cancer Prognosis
The prognosis for esophageal cancer in Australia is similar to other developed countries. The five-year survival rate for esophageal cancer in Australia varies depending on the cancer stage at diagnosis. According to the latest data from the Australian Institute of Health and Welfare (AIHW), the five-year relative survival rate for esophageal cancer is as follows:
- Localised cancer (cancer that has not spread beyond the oesophagus): 39%
- Regional cancer (cancer that has spread to nearby lymph nodes): 19%
- Distant cancer (cancer that has spread to distant organs or tissues): 7%
Note that survival rates are based on population statistics and do not reflect an individual's chances of survival. Many factors can affect an individual's prognosis, including age, overall health, and treatment response. Working closely with your doctor to determine the best treatment plan and monitor the disease's progress is essential.
What if Oesophageal Cancer is Untreated?
If oesophageal cancer is left untreated, it can continue to spread and cause significant damage to the body. This can lead to a range of health complications, including:
- Difficulty breathing
- Malnutrition and dehydration
- Chronic pain
- Esophageal bleeding
- Increased risk of infections
Untreated oesophageal cancer can also be life-threatening, as the cancer can spread to other parts of the body and cause organ failure.
What is Gastric Cancer?
Gastric cancer, also called stomach cancer, is a disease in which malignant (cancerous) cells develop in the lining of the stomach. The stomach is a muscular organ located in the upper abdomen and plays an important role in digestion by breaking down food and passing it to the small intestine. Gastric cancer usually begins in the inner lining of the stomach and can gradually grow deeper into the stomach wall or spread to nearby lymph nodes and other organs.
Most cases of gastric cancer develop slowly over many years. Before cancer develops, pre-cancerous changes often occur in the stomach lining. These changes may include chronic inflammation, thinning of the stomach lining (atrophic gastritis), or abnormal cell growth. Because these early changes rarely cause symptoms, gastric cancer is often diagnosed at a later stage.
Impact of Gastric Cancer on Anatomy and Health
Gastric cancer affects both the structure and function of the stomach. As the tumour grows, it can disrupt normal digestion and interfere with the stomach’s ability to process food.
Some of the ways gastric cancer can impact the body include:
- Stomach wall invasion: The tumour may grow deeper into the stomach wall, affecting its ability to stretch and contract during digestion.
- Obstruction: Large tumours may partially block the passage of food from the stomach into the small intestine.
- Bleeding: Cancer may cause bleeding within the stomach, which can lead to anaemia and fatigue.
- Spread to nearby organs: Advanced gastric cancer can spread to surrounding organs such as the liver, pancreas, or lymph nodes.
- Weight loss and malnutrition: Reduced appetite, early fullness, and impaired digestion can lead to unintended weight loss.
- Systemic effects: In advanced stages, cancer cells may spread through the bloodstream or lymphatic system to other parts of the body.
Because these effects often develop gradually, early symptoms may be mild and easily mistaken for common digestive problems such as indigestion or reflux.
Causes and Risk Factors for Gastric Cancer
Certain factors increase a person’s risk of developing gastric cancer. While the disease can occur in anyone, it is more common in older adults and in individuals with specific medical or lifestyle risk factors.
Common risk factors include:
- Helicobacter pylori infection: Long-term infection with this bacteria is one of the strongest risk factors.
- Chronic gastritis: Ongoing inflammation of the stomach lining may increase cancer risk.
- Family history: A family history of stomach cancer can increase susceptibility.
- Smoking: Tobacco use significantly increases the risk of gastric cancer.
- Dietary factors: Diets high in smoked, salted, or processed foods may contribute to risk.
- Obesity: Excess body weight has been linked with certain types of stomach cancer.
- Previous stomach surgery: Individuals who have had surgery for stomach ulcers may have a slightly increased risk.
- Genetic conditions: Certain inherited syndromes can increase the likelihood of developing gastric cancer.
Understanding risk factors allows individuals and doctors to monitor symptoms and consider screening or early investigation where appropriate.
Symptoms of Gastric Cancer
Early gastric cancer often causes few or no symptoms. When symptoms do appear, they may resemble common digestive conditions, which can delay diagnosis.
Common symptoms may include:
- Persistent indigestion or heartburn
- Upper abdominal pain or discomfort
- Feeling full after eating small amounts of food
- Nausea or vomiting
- Unexplained weight loss
- Loss of appetite
- Difficulty swallowing
- Fatigue due to anaemia
- Vomiting blood or passing black stools (in advanced cases)
Preventing Gastric Cancer
Although not all cases of gastric cancer can be prevented, certain lifestyle and medical strategies can reduce the risk.
Preventive measures include:
- Treating Helicobacter pylori infection: Early diagnosis and treatment of this bacterial infection can reduce inflammation and cancer risk.
- Healthy diet: Consuming a diet rich in fresh fruits, vegetables, and fibre while limiting smoked and heavily salted foods may help protect the stomach lining.
- Avoiding smoking: Stopping tobacco use significantly reduces cancer risk.
- Maintaining a healthy weight: Balanced nutrition and regular exercise support overall digestive health.
- Limiting processed foods: Reducing consumption of processed meats and preserved foods may lower exposure to harmful chemicals.
- Regular medical review: Individuals with a family history of gastric cancer or persistent digestive symptoms should seek medical advice.
Early recognition of risk factors and prompt medical evaluation of symptoms are important steps in reducing the impact of gastric cancer.
Diagnosis of Gastric Cancer
Diagnosis usually involves a combination of medical history, physical examination, and specialised tests.
Common diagnostic methods include:
- Gastroscopy (upper endoscopy): A flexible camera is inserted through the mouth to examine the stomach lining.
- Biopsy: Small tissue samples are taken during endoscopy and examined under a microscope.
- CT scan or MRI: Imaging tests help determine the size of the tumour and whether it has spread.
- Endoscopic ultrasound: Provides detailed images of the stomach wall and nearby lymph nodes.
- Blood tests: These may detect anaemia or other abnormalities.
Accurate staging of the cancer is essential to determine the most appropriate treatment plan.
Treatment for Gastric Cancer
Treatment depends on the stage of the cancer, the location of the tumour, and the overall health of the patient.
Common treatment options include:
- Surgery: Removal of part or all of the stomach (gastrectomy) is the most common treatment for early-stage disease.
- Chemotherapy: Anti-cancer drugs may be used before or after surgery to destroy cancer cells.
- Radiation therapy: High-energy radiation may be used to target and kill cancer cells.
- Targeted therapy: Certain medications specifically target molecular features of cancer cells.
- Immunotherapy: This treatment helps the immune system recognise and attack cancer cells.
What if Gastric Cancer is Untreated?
If gastric cancer is not treated, the tumour will usually continue to grow and may spread to other parts of the body.
Possible complications include:
- Tumour growth: The cancer may grow deeper into the stomach wall and affect normal digestion.
- Stomach obstruction: The tumour may block the passage of food, causing nausea, vomiting, and difficulty eating.
- Internal bleeding: Cancer can cause bleeding in the stomach, leading to anaemia and fatigue.
- Weight loss and malnutrition: Reduced appetite and difficulty eating may result in significant weight loss.
- Spread to other organs: The cancer may spread to nearby organs or distant parts of the body such as the liver or lungs.
Without treatment, gastric cancer can progress and become life-threatening. Early diagnosis and treatment significantly improve outcomes.

